Feeling stuck in the gut confusion of Crohn’s disease vs. Ulcerative colitis? You are not alone. Symptoms blur, names sound similar, and search results can be a maze. This guide cuts through the noise with clear differences, symptoms comparison, and treatment differences Crohn’s vs Ulcerative colitis, so you can have better conversations with your healthcare team.
Crohn’s disease vs. Ulcerative colitis which hits harder
People often ask which is worse. The honest answer, it depends. UC vs Crohn’s severity varies by person, by where inflammation sits, and by complications over time.
- Where it affects, Crohn’s can impact any part of the digestive tract. Ulcerative colitis is limited to the colon and rectum.
- Depth of inflammation, Crohn’s can be transmural inflammation that reaches through the bowel wall. Ulcerative colitis affects the colon lining, the inner surface.
- Pattern, Crohn’s often appears in patches with healthy areas in between. Ulcerative colitis usually spreads in a continuous line starting at the rectum.
- Complications, Crohn’s can cause strictures and fistulas. Ulcerative colitis more often causes rectal bleeding and urgency.
So, which is worse Crohn’s or Ulcerative colitis? Pain, disruption, and risk can be significant with both. What matters most is getting the right diagnosis and plan for you.
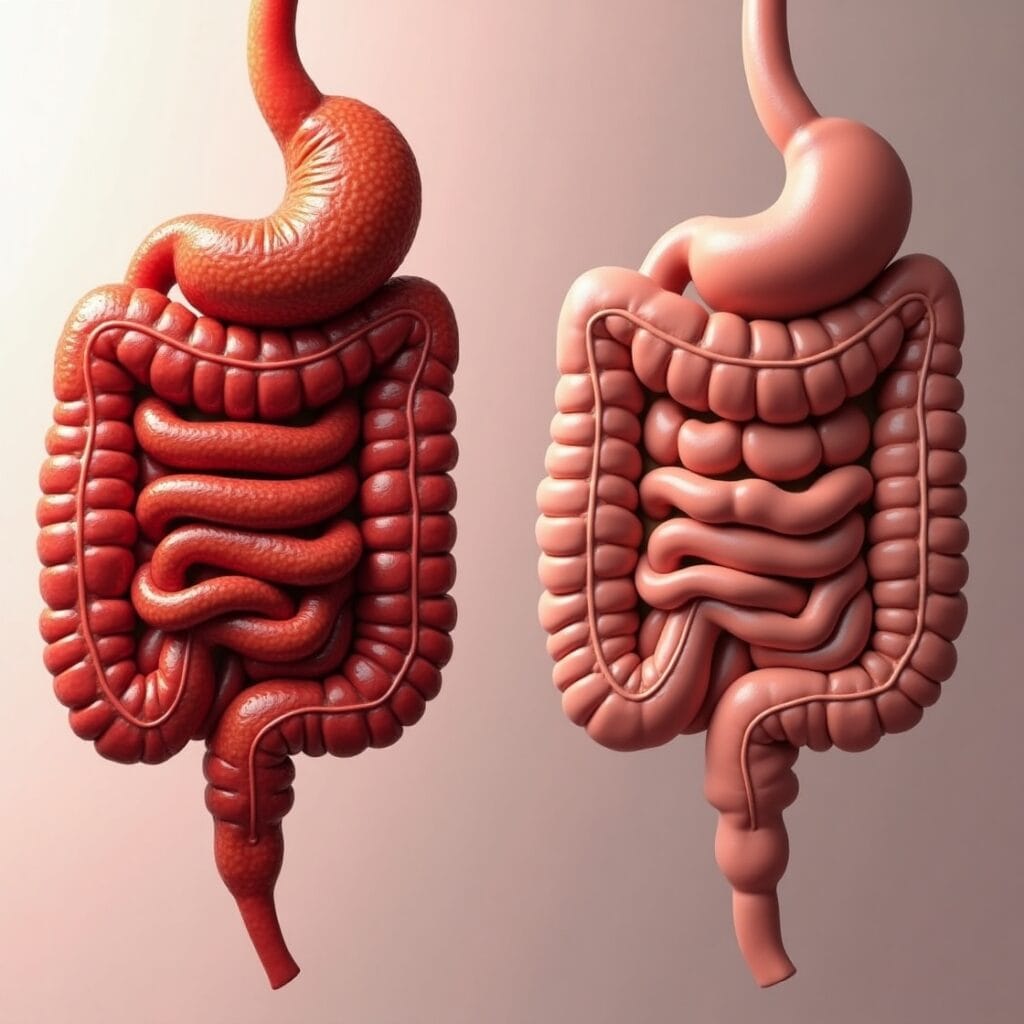
Symptoms comparison Crohn’s vs Ulcerative colitis
There is clear overlap, yet some signals point in useful directions.
- Shared signs, abdominal pain and diarrhoea, fatigue, weight loss, low iron.
- More suggestive of ulcerative colitis, blood in stool, urgency, mucus, pain mainly on the left side.
- More suggestive of Crohn’s, mouth ulcers, pain anywhere in the abdomen, perianal problems, delayed growth in children.
How doctors differentiate
To compare Crohn’s disease and ulcerative colitis properly, clinicians piece together your history with tests. These may include blood tests for inflammation and anaemia, stool analysis to check markers of gut inflammation, endoscopy with biopsies, and imaging such as MRI for small bowel involvement. This evidence helps differentiate between Crohn’s and ulcerative colitis and rules out lookalikes.
Treatment differences Crohn’s vs Ulcerative colitis
Both conditions aim for the same destination, calm the gut inflammation and maintain remission, yet the routes can differ.
- Medicines used in both, steroids for short flares, immunosuppressants, and biologics therapy that targets specific inflammatory pathways.
- More common in ulcerative colitis, 5-ASA drugs may help mild to moderate disease that is limited to the colon lining.
- Surgery, some people with ulcerative colitis choose or need colectomy, which removes the diseased colon. In Crohn’s, surgery treats complications or stubborn segments, it does not remove the underlying tendency for inflammation.
- Faecal microbiota transplantation, still being studied. It shows promise mainly in ulcerative colitis in research settings. Talk to your team before considering any new therapy.
Personalised options and daily tactics
Care is moving toward precision, using tests to match the right tool to the right person at the right time.
- Dietary management, a food and symptom diary can spot patterns, like how fibre, spice, lactose, or caffeine affect you. Ask about targeted approaches during flares versus remission.
- Microbiome analysis and genetic testing, these are being explored to refine choices. Results are one part of the picture, they do not replace clinical judgement.
- Mind and body, cognitive behavioural therapy can reduce stress reactivity and improve sleep, which often softens symptom intensity.
Crohn’s colitis vs ulcerative colitis
Sometimes Crohn’s only affects the colon, this is called Crohn’s colitis. It can look a lot like ulcerative colitis, yet the depth and pattern of inflammation, plus biopsy findings, usually point to the right label. This matters because surgery and long term plans can differ.
Key takeaways
- The difference between Crohn’s disease and Ulcerative colitis is where and how the gut is inflamed.
- Use clues like blood in stool, perianal issues, and urgency as nudges, not final answers.
- Work with your team to differentiate between Crohn’s and ulcerative colitis using colonoscopy, biopsy, imaging, and stool analysis.
- Treatments overlap, yet choices differ by location, depth, and complications.
- Small daily steps help, dietary management, movement, sleep habits, and mental health support.
If you are weighing Ulcerative colitis vs Crohn’s disease and want to compare Crohn’s disease and ulcerative colitis in more depth, take your notes to your next appointment. A short, specific list of questions often gets the best answers.
Medical disclaimer
Remember, This blog post is intended for informational purposes only and should not be construed as medical advice. Always consult with your doctor to discuss your individual situation and determine the best course of treatment for you. Do not start or stop medications without speaking to a doctor. Do not change your diet without speaking to your doctor or a healthcare professional.
Crohn’s can affect any part of the gut and often involves deeper layers. Ulcerative colitis is limited to the colon lining. Patterns and complications differ.
Severity varies by person and by disease location. UC vs Crohn’s severity also changes over time, so individual plans matter most.
They use history, examination, stool analysis, colonoscopy with biopsies, and imaging. The full picture helps confirm the diagnosis.
Both can cause abdominal pain and diarrhoea. Blood in stool and urgency are common in ulcerative colitis, perianal issues lean toward Crohn’s.
Both may use steroids, immunosuppressants, and biologics therapy. 5-ASA is used more in UC, surgery differs between the two.
Dietary management and a food diary can help. Cognitive behavioural therapy can support coping, sleep, and stress.