If you live with Crohn’s, you probably know the symptoms before the menu arrives. Still, the bigger story matters too. The history of Crohn’s disease is full of missed clues, mixed labels, and a few lucky breakthroughs that changed lives. This page brings that story into focus, so the condition feels less mysterious and a bit more manageable.
History of Crohn’s Disease who discovered it
Long before it had a name, doctors were seeing intestinal inflammation without quite knowing what to call it. Early case reports show patterns along the digestive tract that did not fit neatly with known infections or ulcers. People often ask when was Crohn’s disease discovered. The short answer is 1932, in the middle of the Great Depression, when three New York physicians put the pieces together.
In 1932, during Great Depression era medicine, Dr Burrill Crohn, Dr Leon Ginzburg, and Dr Gordon D. Oppenheimer published a landmark paper describing a distinct pattern of disease in the terminal ileum. So, who discovered Crohn’s disease? It was a team effort, grounded in careful pathology and the courage to say this is something new.
How did Crohn’s disease get its name
So, who is Crohn’s disease named after? The condition took Burrill Crohn’s surname largely through historical habit and alphabetical order. In their paper, the trio described what they initially called regional ileitis or terminal ileitis. Over time, Crohn’s disease became the default name, even though inflammation can affect any part of the digestive tract, not just the terminal ileum.
That naming created a neat headline but a messy reality. Crohn’s disease name origin points back to a narrow slice of the gut, while real life is broader and far more stubborn. Today we understand genetic factors and environmental triggers can combine to drive this chronic intestinal inflammation, though the exact mix still varies from person to person.
Why Crohn’s took decades to be properly diagnosed
Before modern tools, diagnosing Crohn’s was like guessing a recipe with your eyes shut. Symptoms overlapped with other conditions, so misdiagnosed Crohn’s disease was common. For years, some people were told it was tuberculosis, ulcerative colitis, stress, or simply an upset stomach that never settled.
Better tools changed the odds. Endoscopy let clinicians see inflammation, ulcers, and strictures directly. Blood tests such as C-reactive protein and erythrocyte sedimentation rate helped signal ongoing inflammation. Imaging improved. Even a quirky balloon dilation test appeared in the historical record, a literal trial of pressure to assess narrowed segments.
The psychology mattered too. Once a label sticks, people tend to see what they expect. That is why Crohn’s disease history includes so many near-misses. Naming shapes attention. If you only look for terminal ileitis, you can miss disease elsewhere along the digestive tract.

Who was Burrill Crohn and why the disease carries his name
Burrill Crohn did not lobby for the limelight. He, Leon Ginzburg, and Gordon D. Oppenheimer were careful observers who noticed a pattern of patchy, transmural inflammation in the terminal ileum that did not behave like tuberculosis or ulcerative colitis. When was Crohn’s disease discovered is answered by their 1932 description of a distinct entity, now tied to his surname.
Their work, and the landmark paper that followed, moved thinking forward. It separated a new condition from lookalikes and opened the door to research on causes and treatments. That moment also set off a century of questions about Crohn’s disease origin and the wider story of inflammatory bowel disease.
As Dr Crohn once wrote, �22This new entity, which I propose to call ‘terminal ileitis,’ may be confused with other diseases of the intestinal tract and may be far more common than the records now indicate.�22 It was a humble warning that misclassification can hide what is right in front of us.
Why Crohn’s was misdiagnosed for decades
Crohn’s was not late to the party, it was wearing the wrong name tag. For years, people were treated for other conditions, sometimes with aggressive surgery, because patterns looked familiar and certainty was scarce. When a picture almost fits, the brain often rounds it up to a match.
Words also steer behaviour. Call something psychological and it gets dismissed. Call it autoimmune and it draws more attention. The same is true here. Once the community narrowed in on terminal ileitis, awareness of disease elsewhere lagged. It took time, improved endoscopy, better imaging, and persistent patient voices to widen the frame.
How common is Crohn’s disease in the UK and what the numbers reveal
Rates have climbed in recent decades, rising from 220 to 400 cases per 100,000 people between 2000 and 2017. And it does not stop there. Projections suggest IBD will affect 1.1% of the UK population by 20251, pushing it closer to a national health crisis than a niche diagnosis.
To put it bluntly, Crohn’s disease statistics in the UK now place us among the top countries globally — second only to the United States2. And while that’s not exactly a podium you want to stand on, it should at least raise eyebrows in public health circles.
What’s more, the condition continues to rise most rapidly among young adults3, raising uncomfortable questions about environmental triggers, diet, and whether anyone in their 20s can ever trust their stomach again. The call for greater awareness, early diagnosis, and better support services has never been louder — or more justified.
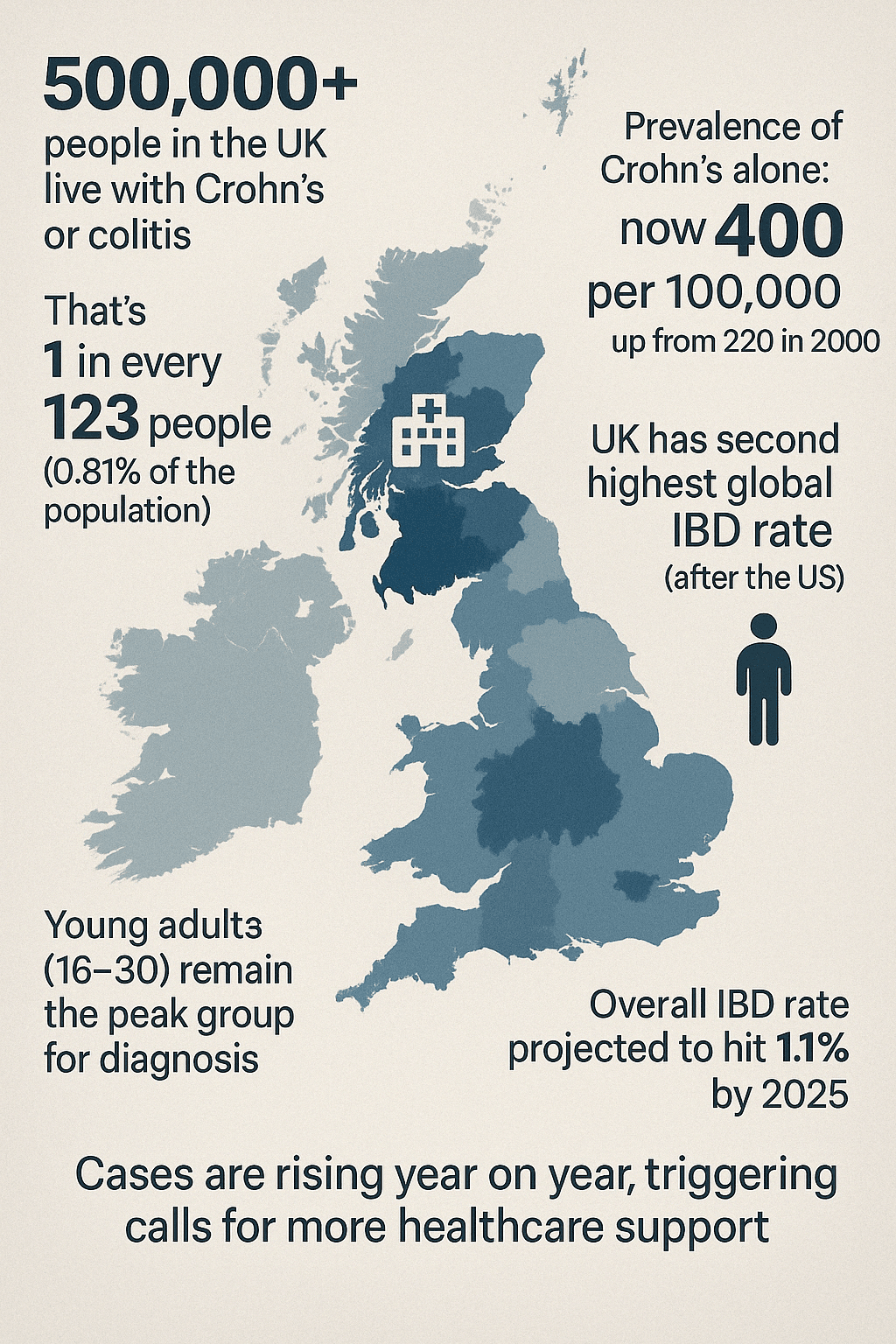
Quick stats on Crohn’s in the UK
- 500,000+ people in the UK live with Crohn’s or colitis
- That is 1 in every 123 people (0.81% of the population)
- Prevalence of Crohn’s alone: now 400 per 100,000, up from 220 in 2000
- UK has second highest global IBD rate (after the US)
- Young adults (16–30) remain the peak group for diagnosis
- Overall IBD rate projected to hit 1.1% by 2025
- Cases are rising year on year, prompting calls for more support
Crohn’s remains a medical riddle wrapped in gut reactions
The history of Crohn’s disease is a reminder that progress often starts with a simple what if we are wrong. That question, asked by Burrill Crohn and colleagues, shifted thinking and improved care for future generations.
If you have Crohn’s, or love someone who does, knowledge really helps. Understanding the 1932 Crohn’s disease discovery, the terminal ileitis history, and the reasons for past medical misdiagnosis can make today’s decisions feel calmer. It is not about dwelling on the past. It is about using it to ask better questions in the clinic.
Remember: This blog post is intended for informational purposes only and should not be construed as medical advice. Always consult with your doctor to discuss your individual situation and determine the best course of treatment for you. Do not start or stop medicines without speaking to a doctor. Do not change your diet without speaking to your doctor or a healthcare professional.
Common questions on the History of Crohn’s Disease
It was first formally described in 1932 by Burrill Crohn, Leon Ginzburg, and Gordon D. Oppenheimer.
It is named after Burrill Crohn, one of the authors on the 1932 landmark paper. He did not seek the naming.
Symptoms overlap with tuberculosis and ulcerative colitis, and early tools could not clearly separate them.
It refers to inflammation in the last part of the small intestine, the terminal ileum, often seen in Crohn’s.
Doctors use endoscopy, imaging, and blood markers like C-reactive protein and ESR, alongside symptoms.
Hundreds of thousands live with IBD in the UK. Crohn’s often starts in young adults.
A 1932 paper defined a new condition. Since then, research has expanded beyond the terminal ileum.